The project ‘Unravelling the mysteries of yersiniosis’ is led by Dr Brent Gilpin at ESR and is funded by the Health Research Council. Maria Hepi from the Social Systems team is working on the social science component of the project, exploring why Māori have low notified rates of yersiniosis.
ESR and Yersiniosis
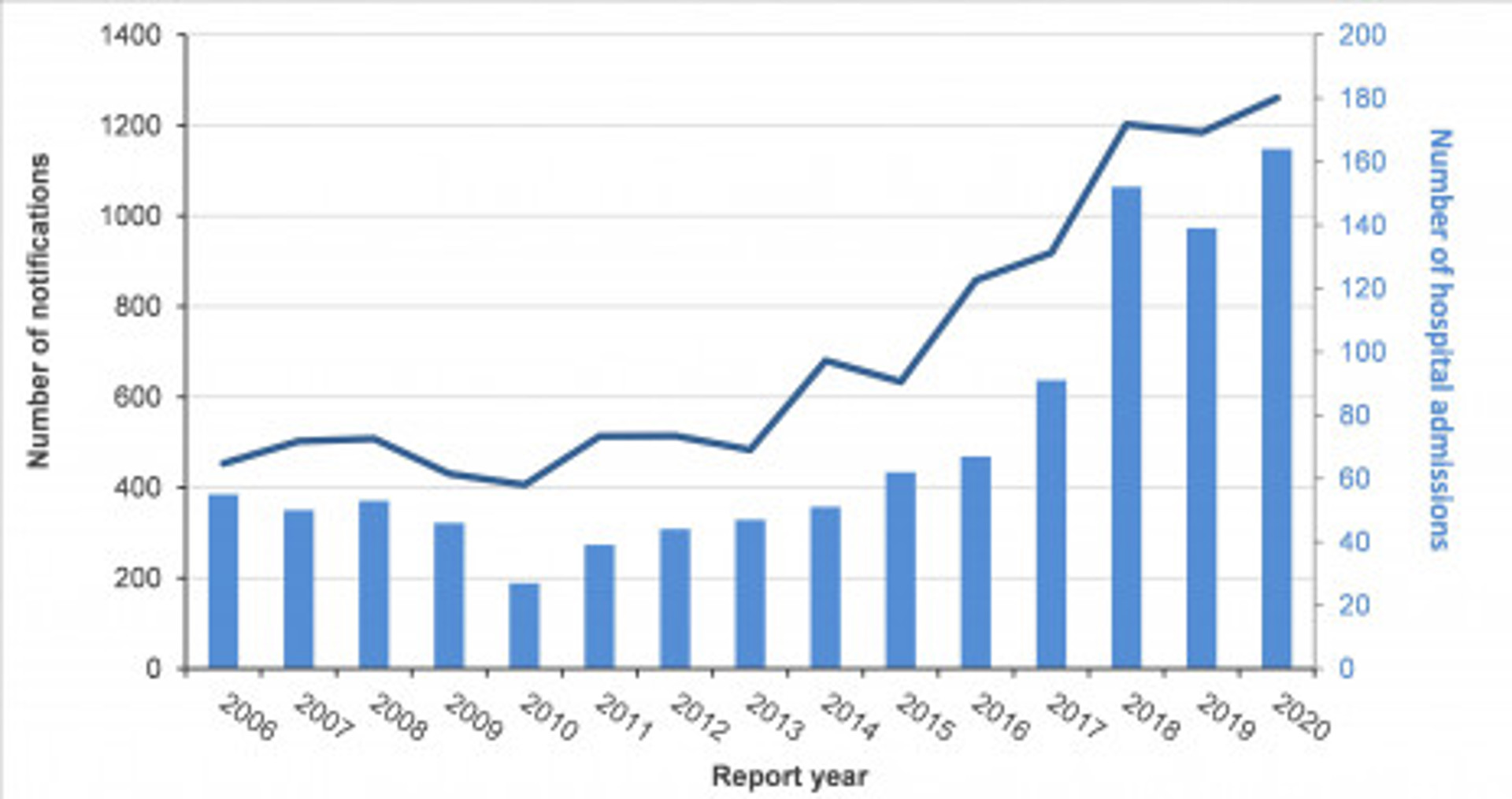
ESR undertakes the surveillance of notifiable diseases(external link) in New Zealand on behalf of the Ministry of Health. New Zealand is seeing a considerable increase in yersiniosis cases and hospitalisations over the last 6 years (Figure 1), but it is not clear as to how people are becoming infected.
Figure 1 (below). Yersiniosis notifications (line) and hospitalisations (bar) by year, 2006–2020 (Horn et al. 2021
Interweaving genomics to learn more about Yersinia enterocolitica
The DNA make-up or whole genome sequence can now be easily determined using state-of-the-art technologies available at ESR. Learn more about genomics.
The bacteria Y. enterocolitica found and isolated from notified individual’s faecal samples, as well as from food, water, animal or environmental samples tested during the project are whole genome sequenced in real-time.
Genomics can help us in many ways
1. Improve public health surveillance
-
Establish whether Y. enterocolitica from clinical cases are genetically related.
We can compare Y. enterocolitica isolates obtained from different people and see if they are genetically related. If they are very closely related then these isolates can be ‘clustered’ and can signal that these people potentially contracted yersinosis from a common source (e.g., food) that can be investigated further.
-
Establish whether a food or source may be contributing to clinical cases
We can compare genomes of Y. enterocolitica from clinical cases with those we find in foods and other sources. Those that are genetically closed related can signal that the food or source may be attributing to clinical cases.
Whole genome sequencing data cannot be used alone. Epidemiological data (i.e., food and source exposure) from clinical cases and/or further investigation is required to confirm a source of infection.
Combining genomic data with the risk-factors data collected in the study will provide robust evidence of key sources contributing the yersiniosis in New Zealand that can be mitigated in the future.
2. Provide information on antimicrobial resistance and virulence
Y.enterocolitica genomes can be searched for genes that are associated with antimicrobial resistance. Comparisons of the genetic data with laboratory quantitative antimicrobial susceptibility assays helps determine whether genomics can be used to predict resistance and potentially guide clinical decision-making.
Genes associated with virulence can also be searched within genomes. Y. enterocolitica Biotype 1A is a controversial type as it is referred to as non-pathogenic internationally, yet this type appears in clinical cases in New Zealand.
We will look at the genomes of all NZ Y. enterocolitica including Biotype 1A to see if there are putative genes that could explain virulence and compare them with laboratory assays and international Y. enterocolitica genomes.
Frequently Asked Questions
What is the Health and Research Council project on Yersiniosis aiming for?
International data suggests that yersinosis is predominately foodborne. Data for New Zealand is lacking or outdated and the key sources and pathways of yersiniosis in New Zealand is unclear.
A case-control study is being undertaken which will help us identify key risk factors, such as certain foods or other possible sources (such as animals or water) that may explain the increase of yersiniosis in New Zealand.
The study focuses on individuals that are notified with yersiniosis within Canterbury, South Canterbury and the West Coast (in collaboration with Community and Public Health. These individuals are telephoned soon after notification and the Canterbury public health unit administer a questionnaire about their risk factors exposures prior to them becoming ill.
The risk-factor data collected from consenting notified cases will be compared to data collected from persons that have not been diagnosed with yersinosis (‘controls’).
We are also testing various foods and other sources (e.g., animals or water) to try and identify whether Y. enterocolitica is present.
The outputs from the study will help us to understand the key causes of yersiniosis so that measures can be put in place to reduce the number of people getting sick in New Zealand.
Determining the burden of illness and severity that yersiniosis is causing in New Zealand
Symptoms of yersiniosis may include diarrhoea and abdominal pain resembling appendicitis. Complications and long-term sequalae such as invasive bloodstream infections and reactive arthritis can also occur.
The burden of the disease and the severity of these symptoms amongst yersiniosis cases in New Zealand is unknown.
Those individuals notified with yersinosis and participating in the study are interviewed about the symptoms and any complications they may be experiencing during and following their illness.
We also are determining whether individuals ill with yersiniosis are visiting the hospital or going to the doctor, whether they are treated with antibiotics and overall establishing how long they feel sick for. We also will investigate whether different types of Yersinia could be causing more severe illness and outcomes.
This data will help us calculate the burden of disease (disability adjusted life years; DALY) that will then use to help with allocating appropriate resources to reduce yersiniosis in New Zealand.
Why do Māori have the lowest notified rate of yersiniosis compared to other Ethnic groups in New Zealand?
Surveillance data indicate that Māori have the lowest notified rates of yersiniosis followed by Middle Eastern, Latin American and African (MELAA) and Pacific peoples (Figure 2) below.
We have a hypothesis that these notification rates severely under-represent the actual disease burden among Māori and Pacific people and that there is under-reporting of yersiniosis and other enteric diseases for Māori, but the reasons are not clear. This research is exploratory and designed to provide insights into current practice and possible service innovations. We expect the results will be able to inform subsequent and larger studies.